Sole pain when walking affects millions of people, from desk workers to athletes, and is often caused by preventable factors. Most people ignore sole pain hoping it goes away, but untreated foot pain worsens over time. The good news: sole pain is usually caused by treatable conditions with clear solutions.
Why Your Sole Hurts
Your foot sole supports 100% of your body weight, plus additional force when you walk. Each foot strike creates impact equal to 1.5 times your body weight; running impact reaches 2-3 times your body weight. The plantar fascia, a thick band of tissue running along your sole, bears the brunt of this stress.
When your feet are overworked, unsupported, or biomechanically compromised, pain develops quickly. Sole pain most commonly occurs in the heel area (plantar fasciitis, heel spurs), the arch (flat feet, arch strain), or the ball of the foot (metatarsalgia, Morton’s neuroma).
Many people wear inadequate footwear with no arch support, have sedentary lifestyles that weaken foot muscles, or increase activity suddenly without proper conditioning. These factors combine to create sole pain that persists without intervention.
Common Causes of Sole Pain When Walking
Plantar Fasciitis
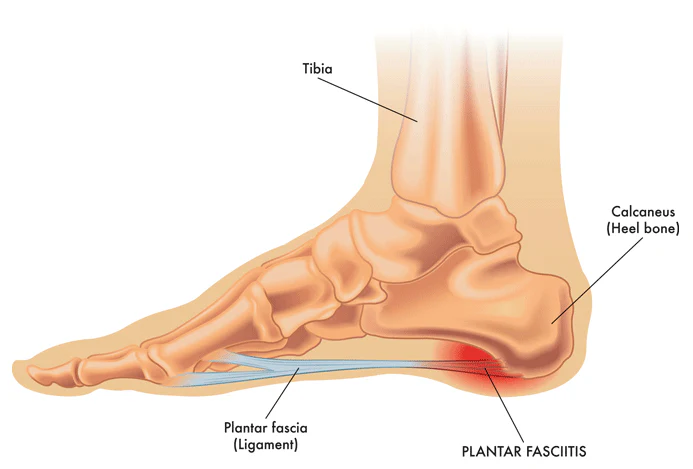
Plantar fasciitis is inflammation of the plantar fascia, the thick tissue band running along your sole. Symptoms include stabbing heel or arch pain which becomes worse in the morning or after sitting, but improving with movement.
Plantar fasciitis commonly affects flat-footed people, runners, people on their feet all day, and those with tight calf muscles. The plantar fascia becomes strained from overuse, tight muscles, or lack of arch support. It accounts for 80% of sole pain complaints, making it the condition you’re most likely experiencing if your sole hurts when walking.
Heel Spurs
Heel spurs are calcium deposits on the heel bone that often develop alongside untreated plantar fasciitis. They cause sharp heel pain, worse in the morning or after activity. Despite what some believe about bone spurs, heel spur pain is completely treatable.
Flat Feet and Fallen Arches
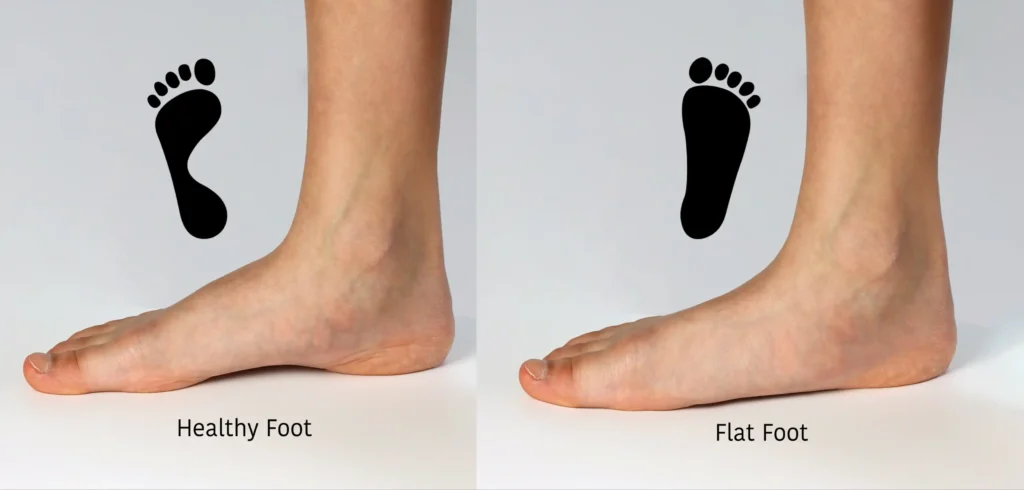
Metatarsalgia is inflammation or pain in the metatarsal area (the area before your toes). Sharp or burning pain in the ball of your foot worsens with walking. It’s commonly caused by high heels, narrow shoes, forefoot striking while running, or high-impact activities that stress the toe joints and require inadequate padding.
Morton's Neuroma
Morton’s neuroma is thickened nerve tissue between your toes that causes sharp, burning pain in the ball of your foot or between your toes, often with tingling. It’s more common in women and progressive if untreated. Risk factors include tight shoes, high heels, and repeated foot stress.
Calluses and Pressure Points
Calluses are hardened skin forming on high-pressure areas of your sole. They hurt when they become inflamed or develop painful cracks. Calluses form from friction caused by poor footwear or bony prominences, often indicating a gait issue that should be addressed.
Foot Strain from Overuse
General foot fatigue and pain from increased activity causes whole-foot soreness that’s worse at the end of the day and improves with rest. Common scenarios include starting a new job requiring you to be on your feet, increasing exercise volume, or vacation walking. This usually resolves with rest and proper footwear; if it persists longer than 2 weeks, seek professional evaluation.
Biomechanical Issues
Overpronation (foot rolls inward excessively), high arches (less shock absorption), tight calf muscles (altering foot mechanics), and weak foot intrinsic muscles (small muscles within the foot that provide support) all contribute to sole pain. Addressing these underlying issues prevents recurrence.
Self-Treatment Relief You Can Start Today
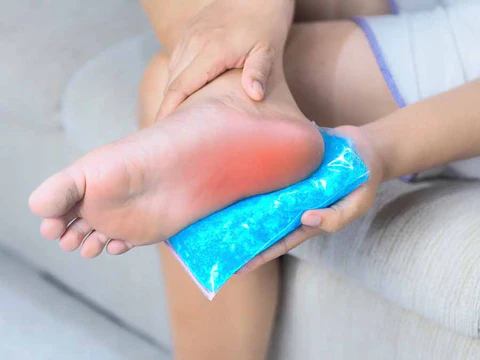
Immediate Relief
Use ice therapy with an ice roller or frozen water bottle under your sole for 15 minutes, 2-3 times daily. Ice reduces inflammation quickly and works best for acute pain or after increased activity.
Reduce walking and standing if possible. Avoid high-impact activities like running or jumping temporarily. Elevate your feet to reduce swelling.
Change your footwear immediately. Wear supportive shoes with adequate arch support, avoiding flat shoes, flip-flops, and worn-out soles. Cushioned insoles or over-the-counter orthotics provide immediate relief for many people.

Short-Term Care (Days 2-7)
Perform stretching daily. Calf stretches (tight calves stress the sole) should be held for 30 seconds, 2-3 times daily. The plantar fascia stretch involves sitting, pulling your toes toward your shin, and feeling the stretch along your sole. Lean forward against a wall for your Achilles stretch, feeling the stretch in your calf.
Strengthen your feet with towel curls. Curl your toes to scrunch a towel across the floor to strengthen foot intrinsic muscles. Do calf raises in 3 sets of 15, building strength gradually. Activate your arch by walking barefoot on uneven surfaces like sand or grass to engage foot muscles.
Roll and massage using a massage ball or foot roller along your sole, focusing on tender areas. Roll your foot over a tennis ball or lacrosse ball for 10 minutes daily. Gentle self-massage to tight spots in your arch and heel helps significantly.
Take ibuprofen or naproxen as directed to reduce inflammation. Stay hydrated and eat anti-inflammatory foods like fish, berries, and leafy greens to support tissue healing.

Long-Term Management (Week 2+)
Invest in proper footwear. Supportive athletic shoes or orthopedic shoes with good arch support and cushioning prevent recurrence. Avoid cheap flip-flops, worn-out shoes, and completely flat shoes.
Consider orthotics. Over-the-counter options work for many people, while custom orthotics prescribed by a physiotherapist or podiatrist address persistent issues by correcting biomechanics and preventing recurrence.
Modify your activity gradually. Increase walking or activity with proper footwear. Avoid sudden increases in activity level. Cross-train with low-impact activities like swimming or cycling if foot pain limits other options.
| Pain Location | Likely Cause | Best Home Treatment | Recovery Timeline |
|---|---|---|---|
| Heel | Plantar fasciitis | Ice, stretching, supportive shoes | 2-8 weeks |
| Arch | Flat feet or strain | Arch support, strengthening | 1-4 weeks |
| Ball of foot | Metatarsalgia | Padding, shoe changes, rest | 1-3 weeks |
| Whole sole | General overuse | Rest, ice, footwear | 1-2 weeks |
| Between toes | Morton's neuroma | Wider shoes, padding | 2-4 weeks |
| Localized tender spot | Callus or pressure point | Padding, moisture, gentle care | 1-2 weeks |
When to See a Physiotherapist
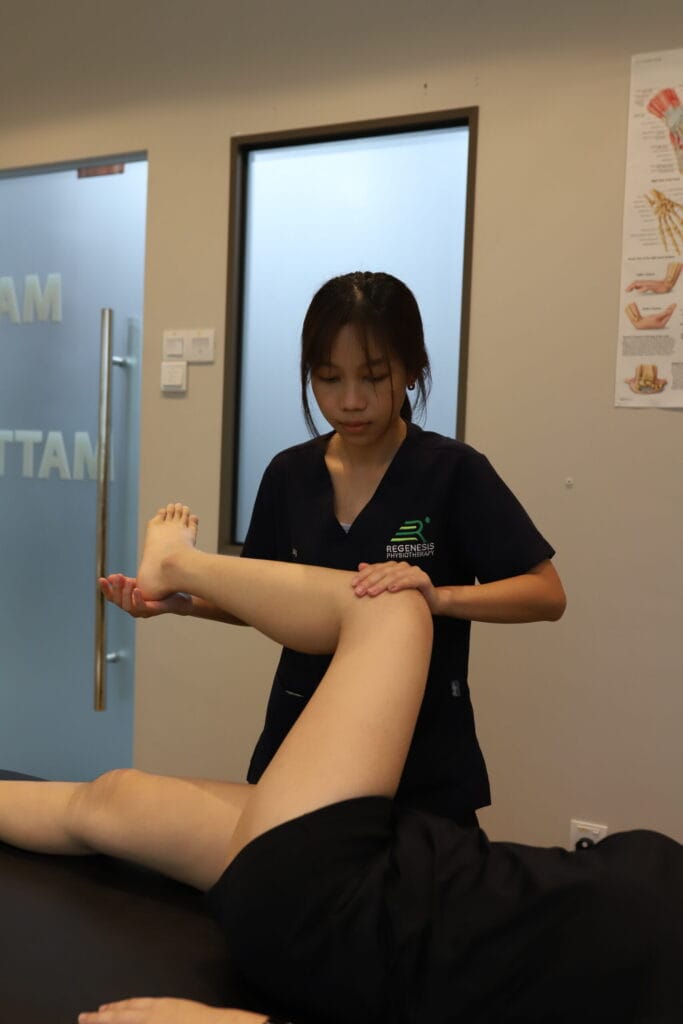
A physiotherapist performs comprehensive foot and gait assessment, identifying the biomechanical issues causing your pain. They evaluate your arch, foot strike pattern, calf flexibility, and foot strength. They prescribe targeted foot-strengthening and flexibility exercises specific to your condition. They may recommend or adjust orthotics based on your biomechanics. They teach proper footwear selection for your foot type. They create a progressive return-to-activity plan if pain is activity-related.
You can consider seeing a physiotherapist if:
- Your sole pain persists beyond 2 weeks despite home treatment
- Pain significantly impacts your walking or daily activities
- You’re unsure of the exact cause and need professional assessment
- You have recurring sole pain (indicating an underlying biomechanical issue)
- You want to prevent future foot pain and understand your gait patterns
- Pain is related to running, sports, or athletic activity
- You need gait analysis to correct walking or running mechanics
- You’re wearing orthotics but still experiencing pain
Unlike generic advice, physiotherapy addresses the root cause of your sole pain. If your pain stems from weak intrinsic foot muscles, they’ll strengthen them. If it’s from tight calves, they’ll address mobility. If it’s from overpronation, they’ll correct your mechanics.
Relieve Sole Pain with Regenesis Physiotherapy

Sole pain when walking is common but treatable. Most cases resolve with rest, proper footwear, stretching, and strengthening exercises. By identifying the cause of your pain and implementing appropriate treatment, you can return to pain-free walking.
Start with self-care strategies and invest in supportive footwear. If pain persists beyond 2 weeks or significantly impacts your walking, a physiotherapist can assess your biomechanics, identify the root cause, and prescribe targeted solutions.