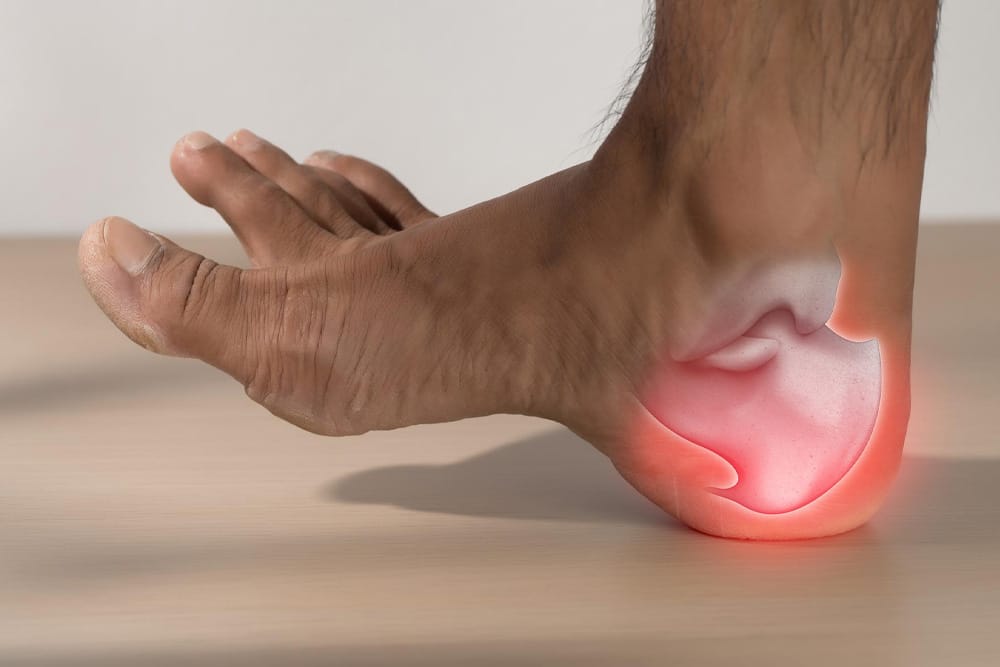
Plantar fasciitis is pain in your heel or arch caused by stress on the plantar fascia, the tissue band running along the bottom of your foot. What x-rays won’t show you is that your fascia is being overworked and inflamed because something else isn’t working right.
This condition is very treatable if you address the root cause, not just the pain. Most people try rest, ice, and expensive orthotics without addressing why the plantar fascia is stressed in the first place. Physiotherapy treats the actual cause, from tight calves and weak foot muscles to bad habits, to make sure pain doesn’t come back.
Plantar Fasciitis Causes
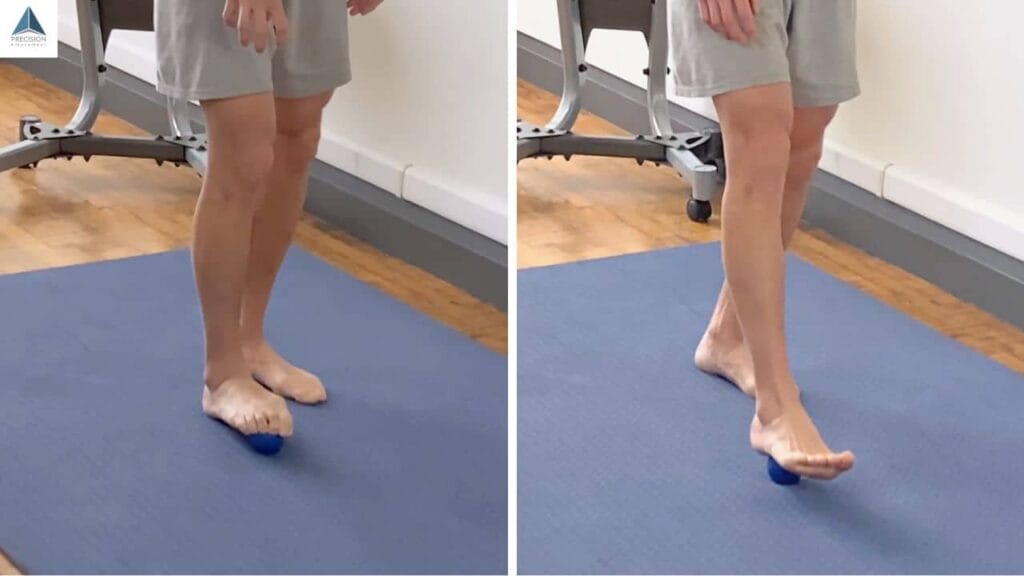
Tight calf muscles are the most common cause of plantar fasciitis. Your calf muscles connect to your plantar fascia through your heel, so when your calves are tight, they pull on the fascia and create stress and pain. This tightness builds gradually from running, standing jobs, or simply not stretching.
Weak foot muscles also contribute significantly. Your foot has small muscles that support your arch. When these muscles are weak, your arch collapses slightly, stressing the fascia. Weakness develops from wearing supportive shoes that do all the work for your feet, preventing your muscles from getting stronger.
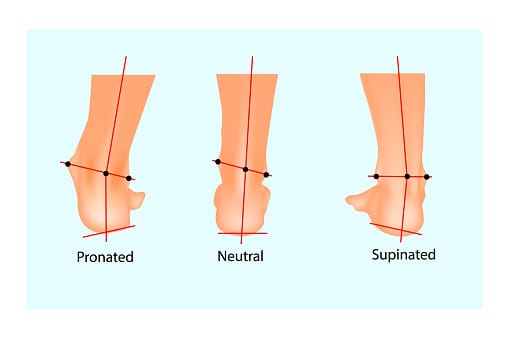
Poor foot mechanics like overpronation (your foot rolling inward excessively) stresses the fascia, as do flat feet or fallen arches that provide poor support. Walking or running with poor form increases the load on your plantar fascia.
Weak glutes and hip muscles are often overlooked. These muscles change how you walk, increasing stress on your feet. Poor hip stability forces your body to compensate, and those compensations often end up stressing your plantar fascia.
Activity and lifestyle factors also play a role including:
- Sudden increases in running or standing
- Poor footwear (e.g. flat shoes, flip-flops without arch support)
- Lack of stretching and conditioning
- Tight hip flexors from sitting all day
Plantar Fasciitis Symptoms
Plantar fasciitis usually starts with a sharp or stabbing pain in your heel, especially in the morning when you first get out of bed. Pain often improves as you move around but comes back after you rest.
Other early warning signs include:
- Pain that goes away with rest but returns when you’re active again
- Stiffness in your foot after sitting for extended periods
- Pain worse with barefoot walking on hard surfaces
As the condition develops, symptoms become more noticeable. You experience severe heel pain that limits how far you can walk or how long you can stand. Pain continues to persist or even worsens with rest. You might see swelling or inflammation under your foot with certain shoes becoming too painful.
Most people experience early warning signs for weeks before seeking help. The earlier you address plantar fasciitis, the faster it responds to treatment. If you’re feeling any heel or arch pain, this is your signal to start stretching and strengthening before it becomes a serious problem.
Plantar Fasciitis Physiotherapy Exercises and Treatment
Physiotherapy for plantar fasciitis works because it combines immediate pain relief through stretching and massage with progressive strengthening that addresses the root causes. You’ll do stretching and strengthening exercises simultaneously, with stretching providing relief while strengthening prevents the problem from returning.



Calf Stretches
Calf stretches are the foundation of treatment. Tight calves are responsible for most plantar fasciitis cases, making calf stretching the most important exercise you can do. Do these 3-4 times daily, especially before bed and first thing in the morning.
Standing calf stretch: Lean against a wall with your back leg straight behind you. Feel the stretch in your calf. Hold for 30 seconds, repeat 3 times. Do this 3-4 times daily.
Soleus stretch: Use the same position but bend your front knee slightly to target the deeper calf muscle. Hold for 30 seconds, repeat 3 times. Do this 2-3 times daily.
Foot Strengthening Exercises
Activation exercises wake up the small muscles inside your foot that support your arch. These exercises might seem small, but they rebuild the strength in your foot that supports your arch and reduces fascia stress.
Towel curls: Sit barefoot with a towel on the floor in front of you, then curl your toes to scrunch the towel toward you. Do 3 sets of 10 reps. This strengthens the bottom of your foot.
Short foot exercises: Sit or stand and try to shorten your foot by making your arch higher without curling your toes. Hold for 5 seconds, repeat 15 times. Do this 2-3 times daily.
Arch strengthening progresses the treatment once you’ve done initial stretching and massage work.
Hip and Glute Strengthening
Hip and glute strengthening address the bigger picture of your foot pain. Weak glutes change how you walk, adding stress to your plantar fascia. Include these exercises 3-4 times weekly.
Single-leg glute bridges: Lie on your back with one leg extended and lift your hips using your glutes. Do 3 sets of 12 reps each leg. This corrects gait patterns that stress your feet.
Clamshells: Lie on your side with your knees bent and open your top knee against resistance. Do 3 sets of 15 each side. This stabilizes your hips, improving walking mechanics.
How Long Does Plantar Fasciitis Treatment Take?
Most people notice pain relief within 2-4 weeks of consistent stretching and strengthening. During weeks 1-2, daily calf stretches and foot massage provide noticeable pain relief. Weeks 2-6 are the strengthening phase when pain continues to decrease as your foot muscles strengthen and your walking mechanics improve. By weeks 6-12, most people are pain-free or nearly pain-free. Beyond that, ongoing daily stretching and weekly strengthening prevent recurrence.
Recovery speed depends on how long you’ve had pain. Early intervention—treating plantar fasciitis within 1-2 weeks of first noticing pain—means faster recovery. Long-standing plantar fasciitis that you’ve had for months or years takes longer to resolve, but it still responds well to physiotherapy. Be patient with the process; the exercises are addressing the root cause, which takes time.
FAQ on Plantar Fasciitis
Yes, stretching and gentle strengthening are fine even with pain. Avoid high-impact activities like running and jumping until you're pain-free with normal walking. Pain should decrease over time with consistent exercise, not increase. If exercises increase pain, reduce intensity or modify the movement.
Your foot shortens and the plantar fascia tightens overnight. Morning pain is completely normal. Do calf stretches before getting out of bed, and pain usually improves once you've moved around and your fascia has warmed up.
See our physiotherapist for professional assessment. They may identify issues you're missing like overpronation, gait problems, muscle imbalances, or movement patterns you haven't noticed. Professional guidance can speed up recovery and ensures you're doing exercises with proper form, which makes a big difference in results.
Yes, if you stop stretching and strengthening. Once recovered, maintain daily calf stretches and weekly strengthening as part of your routine. This prevents recurrence and keeps you pain-free long-term.
Get Plantar Fasciitis Treatment with Regenesis' Sports Physiotherapy

Most plantar fasciitis cases resolve completely with proper physiotherapy treatment. At Regenesis Physiotherapy, our specialists can create a treatment plan that gets you back on your feet. You’ll understand exactly which muscles are tight or weak, how to train smarter, and how to move without pain. Get back to walking, running, and living pain-free.